Diagnosis
PsA can be difficult to diagnose, partly owing to the fact that its common symptoms look similar to other conditions, particularly other types of arthritis. Diagnosis is commonly made by identifying inflammation in joints, entheses (the sites where tendons, ligaments, and joints attach to bone) or the spine, when there is also psoriasis of skin and/or nails present. Importantly, for PsA diagnosis, rheumatoid factor will be absent in blood tests. This is a key difference between PsA and RA.
During your exam, your doctor is likely to:1

Testing
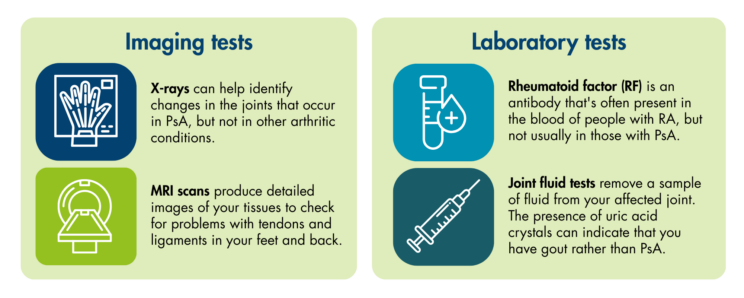
There is no specific test that can confirm a diagnosis of PsA. However, it can be helpful to conduct tests which rule out other causes of joint pain, including RA. The types of tests are shown here:1
Although there is no specific test to diagnose PsA, in 2006 the Classification Criteria for Psoriatic Arthritis (CASPAR) criteria were published,2 helping doctors to define PsA when enrolling patients into clinical trials. The guidelines can be used to support clinicians when making a diagnosis.
The criteria include a list of signs and symptoms, which are assigned scores. If the patient scores 3 or more points, they could have PsA.

References
- Psoriatic arthritis – Mayo Clinic. Available at: https://www.mayoclinic.org/diseases-conditions/psoriatic-arthritis/diagnosis-treatment/drc-20354081. Last accessed April 2025.
- CASPAR Criteria - Psoriatic arthritis – WebMD. Available at: https://www.webmd.com/arthritis/psoriatic-arthritis/caspar-criteria-psoriatic-arthritis. Last accessed April 2025.


